Concussion Recovery: Beyond Arbitrary Timelines
By Associate Professor James McLoughlin
The recent Herald Sun article1, based on a new Swinburne University study using transcranial magnetic stimulation (TMS)2, highlights what many clinicians have long recognised: concussion recovery is not as simple as counting down the days.
In sport, return-to-play (RTP) rules are often based on arbitrary timelines; 12 days in elite AFL, 21 days in community levels, rather than an accurate picture of brain recovery. This study found that while athletes reported feeling symptom-free after about 12 days, measures of cortical inhibition (via TMS) were still abnormal for up to 26 days.
Every day in Australia, we hear that an athlete is sidelined due to “concussion protocols”, rather than what is really happening; the athlete is recovering from a concussion injury. Concussion is a rapid head acceleration injury with neurophysiological, musculoskeletal, and psychological consequences. Just like a hamstring or shoulder injury, recovery requires an individualised, multimodal assessment, not an arbitrary timeline. You don’t hear of players out with “hamstring protocols”, they are recovering from a hamstring injury. And running without pain symptoms certainly does not mean you have fully recovered!
This reinforces what we see clinically every week: symptom resolution does not necessarily mean full recovery.
Research Tools vs. Clinical Reality
I have followed TMS research closely for over two decades. It provides fascinating insights into brain physiology, but I remain cautious about its role in clinical decision-making. The same caution applies to other emerging research tools, like visual evoked potentials (VEPs), which are currently being pitched as clinical aids but are still largely investigational3.
These technologies give us another lens into brain recovery, but the reality is that a comprehensive clinical assessment still provides the most meaningful guidance for safe RTP decisions.
Interestingly, this very study also included a smooth pursuit oculomotor test and the recovery timelines it revealed were remarkably like those detected by TMS (see Figure 1 & 2)2. This illustrates that clinical tools already in use can provide equivalent and actionable insights.
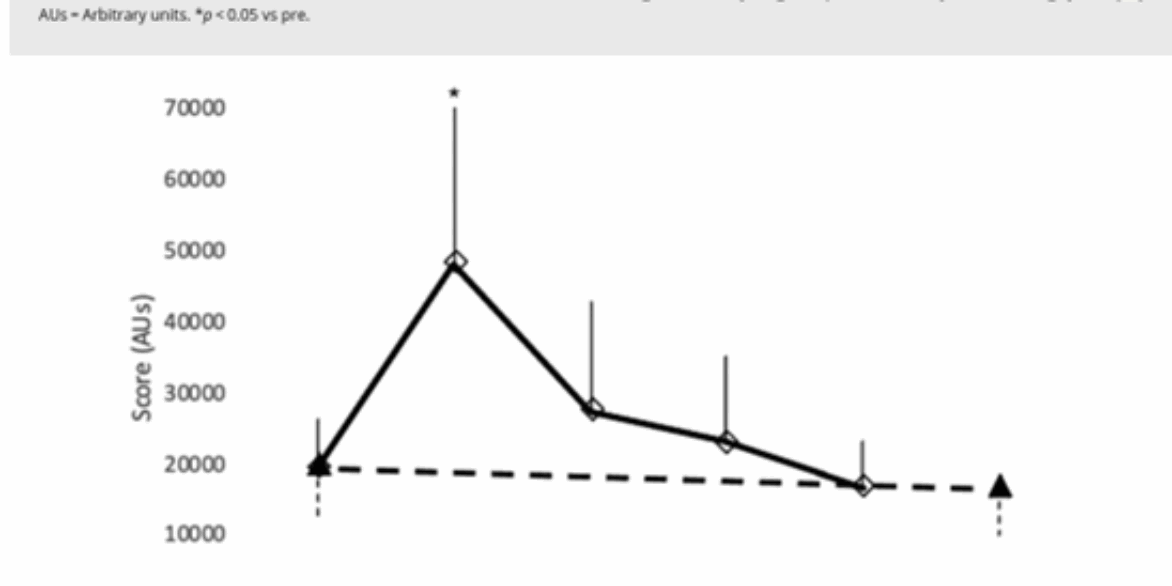
Figure 1
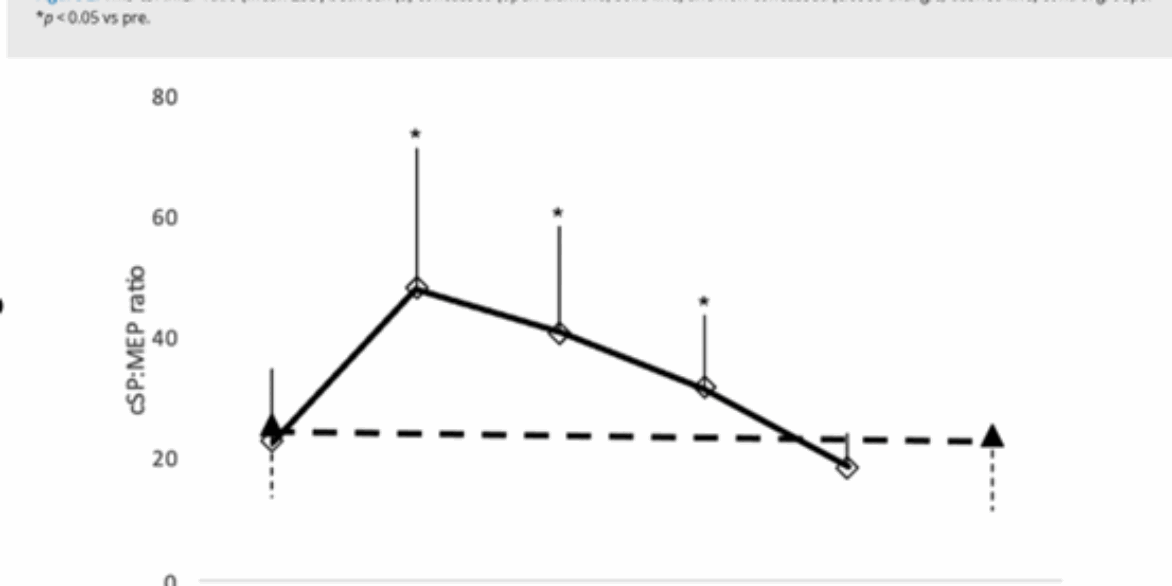
Figure 2
The Power of Multimodal Clinical Screening
Within our global Your Brain Health (YBH) network, oculomotor smooth pursuit testing is already routine. But it’s just one piece of a much larger puzzle. Clinicians in our network use a multimodal screen that assesses:
- Smooth pursuit, saccades, anti-saccades, gaze stability, and optokinetic movements with Neuroflex®.
- Objective measures of postural sway, balance and vestibular signs & symptoms
- Cognitive functions such as attention, memory, and processing speed
- Mental health, sleep, and confidence
- Coordination and broader motor control, including cervical spine contributions
- Relevant medical history and contextual factors
This multimodal approach provides a clear, real-world picture of recovery—and directly informs decisions about returning to play, learn, and work. The idea that symptom recovery alone does not align with objective markers is not new. In fact, defining recovery purely in terms of symptom resolution has been one of the greatest flaws in concussion research to date.
Why This Matters
Every athlete deserves recovery care that is:
- Individualised – no two concussions recover the same way
- Comprehensive – covering brain, body, and psychological health
- Transparent – so players, families, and clinicians can track progress together
This is one of the reasons we built ScreenIT, software that integrates all these clinical measures, streamlining care for the individual while also creating robust, longitudinal datasets to advance concussion research.
Moving Forward
The Swinburne study is important because it reinforces that relying on symptoms—or arbitrary timeframes—alone is not enough. But rather than waiting for research tools like TMS or VEPs to become clinically viable, we already have the ability to perform comprehensive, multimodal assessments that guide safer recovery today.
By combining best-practice measures with emerging technologies, we can ensure athletes return not just when they feel ready, but when their brains and bodies are truly ready to perform at their best.
Bottom line: Concussion recovery should not be dictated by the calendar. Neurophysiological tools like TMS and VEP provide useful insights, but the cornerstone remains a comprehensive, multimodal clinical assessment—supported by technology like ScreenIT and delivered by skilled clinicians who understand the complexity of brain health.
References
- Clarke, B. (2025, August 17). When do you recover from a concussion? Shock new findings. Herald Sun. https://www.heraldsun.com.au/health/mental-health/concussion-recovery-periods-may-be-too-short-new-brain-study-suggests/news-story/73aa4cf85aa55e875b42c3497f96651b
- Pearce, A. J., Middleton, K., & Clarke, A. (2025). Time-course responses following sports-related concussion: a multi-modality study. The Physician and Sportsmedicine, 00913847.2025.2541579, 1–9.
- Fong, D. H. C., Cohen, A., Boughton, P., Raftos, P., Herrera, J. E., Simon, N. G., & Putrino, D. (2020). Steady-state visual-evoked potentials as a biomarker for concussion: A pilot study. Frontiers in Neuroscience, 14, 171.
